The state of the health services in Ethiopia
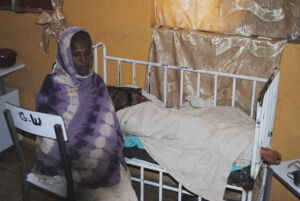
Our structural analyses of the Ethiopian health services and the hospitals in Bishoftu, Axum, Aduan, Mekele, and Addis showed that not all parts of the population have access to health care facilities.
Ethiopia’s public health services comprise the following facilities:-
- Central referral hospitals
- Regional hospitals
- Rural hospitals
- Health Centers
- Health stations, clinics
- Health posts
These hospitals and facilities are state-run. They are allocated an annual budget. This budget has to pay for all expenses: Personnel, materials, treatments. It is controlled by the federal health department and health offices.
Additional health care services are provided by the private sector:-
- Hospitals and private clinics
- Pharmacies
- Facilities run by NGOs or religious groups/charities
- Traditional healers
Depending on their income, patients are charged for their hospital treatment. Only those with at least a modest income can afford to come here. People with higher earnings opt for private medical care. Some private care can cost less than that at state-run clinics. People without any income use health centers or health stations, if nearby. The care they offer varies and they can be somewhat unpredictable. Anyone visiting outside opening hours may be turned away or find the facility closed. There is no organized emergency cover as is common in European countries.
Ethiopia has no general health insurance system. However, there is a state-run health insurance for the 15,000 or so civil servants. The few private insurers that do exist only provide cover for a tiny fraction of Ethiopia’s population. Most people have to pay for health care themselves. For the very poor, as most Ethiopians are, a voucher scheme is available from their local authorities. This entitles them to free but very basic medical treatment.
Treatment is charged separately for examinations, medications, surgery, accommodation, care, food and drink, etc.
The ratio of doctors to population in Ethiopia is far lower than in the west. Services normally performed by doctors in the west are frequently carried out by so-called health officers. These include wound treatment, obstetrics, including cesarean sections, AIDS treatment, tuberculosis treatment, and more.
Most doctors work for state-run hospitals. Their income is too low to live on. Hence, most physicians also run their ‘private clinics’. Varying from region to region, they spend a considerable part of their time working in their own facilities.
In Ethiopia, hospital beds are scarce. Still, empty beds can be found in almost all hospitals. The reasons for this are shortages, both in personnel and materials.
Medical personnel such as doctors, nurses, carers and health officers are frequently very well trained, and their practical experience compares surprisingly well to European standards. However, there is a severe shortage of technical personnel. As a result, medical equipment is poorly maintained and often rendered useless when defective. In many clinics, expensive machinery sits idle because of minor defects or manuals written in a foreign language.
While on an evaluation and repair mission in the north of the country in January of 2011, two of our engineers managed to get numerous machines such as autoclaves, breathing apparatus, anesthesia apparatus and other lab equipment up and running again that had been out of action due to trivial defects. Their mission was to pass on skills and train up technical personnel for the maintenance of such equipment. They found no one to train.
More often than not, machines in hospitals only work as long as NGO staff looks after them. In Aduan, an X-ray machine was installed and maintained by a Norwegian NGO for a number of years. Following their departure, the equipment gradually fell into disrepair, with features like fluoroscopy and automatic development failing. Today, it can only be used for simple exposures.
The most predominant health problems in Ethiopia are infectious diseases, e.g. malaria, tuberculosis, worm infection, leishmaniasis, schistosomiasis, diarrhea, infection of the upper and lower respiratory passages, asthma, skin diseases and HIV/AIDS-related infections, eye diseases, e.g. trachoma, and epilepsy. Also significant are accidents due to increased road traffic, as well as domestic accidents such as fractures and impalements. Perinatal mortality in children (2005: 109/1,000 live births) and mothers (8%) is very high.